We are your trusted advisors, focused on creating unique solutions and superior employee benefit outcomes, while improving the health and well-being of plan participants.
Who We Are

Webber Advisors is a full-service employee benefits consulting firm, but we are not just here to help you pick an insurance plan. Webber Advisors believes in innovation that makes your job easier and provides the solutions you need. We have narrowed this into three fundamental principles: we believe every employer should have a population health strategy, be compliant and offer a superior employee experience.
Learn MoreWhat We Do
At Webber Advisors, we understand that making decisions regarding your employee benefit programs and services can be overwhelming. We also know it can be a leap of faith when finding a trusted partner to help guide you through the often-times challenging process. Here at Webber Advisors, we are committed to finding the RIGHT solution for you and not just selling a product or service. As such, we employ the following key principles that embody the overarching goals and values of Webber Advisors:
Who We Serve
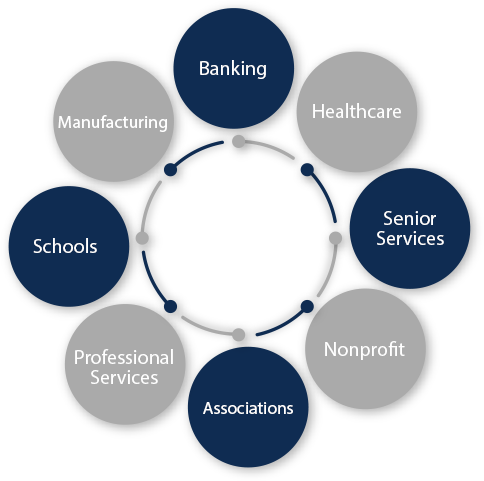
For nearly 50 years, we have maintained a robust client base, representing a diverse group of dynamic professions. We have served broad array of banking institutions, healthcare and senior services providers, nonprofit organizations, associations, schools, manufacturers, and professional services organizations. We pride ourselves in being your strategic advisor, becoming knowledgeable in your core business so that we can align you with the best possible solutions.
We Love Our Clients! They Love Us!
Duncansville
1644 Plank Road Duncansville, PA 16635 (814) 695-8066
Altoona
3107 Beale Ave., Suite 101 Altoona, PA 16601 (814) 944-5028
Greensburg
233 W. Pittsburgh St. Greensburg, PA 15601 (724) 837-8250









